This year has been a great year so far for research into the possibility of non-celiac gluten sensitivity. Most exciting, Stephan Guyenet is now reporting the survey results of participants in Matt Lentzner's Gluten-Free January (see part I and part II). I'm especially glad that of all people this survey fell into Stephan's hands, because like few other scientists I believe he'll treat the data very fairly, treating hypotheses optimistically while also honestly recognizing the limitations of the data, as part I has already proved. The Wall Street Journal also recently gave the topic some attention, and a new double-blind, randomized, placebo-controlled trial recently provided some very weak evidence supporting the phenomenon's existence.
That trial will be the main subject of this post. I was going to title the post "New Study Provides Incredibly Weak But Nevertheless Supportive Evidence that Gluten Might Cause Problems in Some Non-Celiacs If It Has Been Chemically Modified to Resemble the Inside of a Celiac's Intestines," but I thought I'd go with something less sarcastic in order to offer a more constructive attitude in a field that desperately needs — and deserves — more research.
So let's take a look at that study.
Researchers from the Department of Medicine and Gastroenterology at Monash University in Australia published it in the American Journal of Gastroenterology. They gave it the title, "Gluten causes gastrointestinal symptoms in subjects without celiac disease: a double-blind randomized placebo-controlled trial." Their overall conclusion in the abstract is a fair summary of their research:
"Non-celiac gluten intolerance" may exist, but no clues to the mechanism were elucidated.
I have no doubt in my mind that many people do not tolerate wheat. And I think it is a very reasonable and deserving hypothesis that some of this intolerance may be due to gluten. But much of it may not, as there are other things in wheat that could potentially be a problem. Automatically attributing all wheat intolerance to gluten is likely to hamper someone's ability to resolve any residual health problems they might have, because a better and more accurate understanding of just what they are reacting to might help them more easily identify other foods that are a problem.
This new Australian study is, to my knowledge, the first well controlled study demonstrating harmful effects from consuming wheat gluten in live people without celiac. The study was conducted extremely well, although the reporting of the data was poor and the effects were not very impressive.
One of the strengths of the study is that the investigators actually controlled for the possibility of intolerance to non-gluten aspects of wheat by adding pure gluten to gluten-free muffins and bread. They randomly allocated half the subjects to a group that ate the gluten-free muffins and bread with nothing added, and the other half to a group that ate the same muffins and bread but with 16 grams per day of pure gluten added.
They were particularly concerned about fructans, which include the shorter-chain fructooligosacharides and the longer-chain inulin, and they cited a study showing that both fructose and fructans induce symptoms in patients with irritable bowel syndrome.
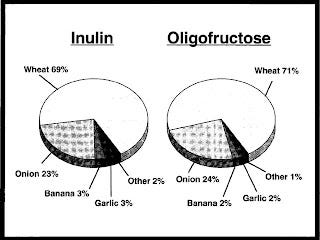
The main source of fructans in the American diet is wheat:
Moshfegh AJ, Friday JE, Goldman JP, Ahuja JK. Presence of inulin and oligofructose in the diets of Americans. J Nutr. 1999;129(7 Suppl):1407S-11S.
As Stephan pointed out, a good way to tell if you don't tolerate fructans well is if you don't do well with onions. Other sources include bananas, asparagus, chicory root, dandelion greens, garlic, globe artichoke, Jerusalem artichoke, leeks, barley, and rye. Out of these, bananas, globe artichokes, and the non-wheat grains contain the least.
Unfortunately, a study's greatest strength can sometimes also be its greatest limitation. It turns out that the gluten used in this study was deamidated.
As I pointed out in my last gluten post, "Wheat: In Search of Scientific Objectivity and New Year's Resolutions," this is the process that normally occurs in the intestine of someone who has celiac disease. The enzyme tissue transglutaminase ordinarily does not exist inside the intestinal lumen, but when the intestine suffers tissue damage, cells release it. The enzyme's molecular action is to convert the amino acid glutamine to the amino acid glutamate within proteins in order to cross-link proteins as part of the tissue repair process. However, it also manages to make a gluten fragment immunoreactive. This fragment stimulates the immune reaction in celiac disease only after being deamidated, which suggests that there may be something besides gluten, such as a virus or some other pathogen, that may be involved in causing intestinal damage before the reaction to gluten actually sets in. However, once celiac gets going this enzyme hangs around perpetually, since celiac involves perpetual intestinal damage.
So this gluten, it turns out, was chemically deamidated instead.
How did I find this out? Well, first I looked at the company's web site. The actual product used in the study, GemTec 1160, was nowhere to be found. It turns out that the company no longer makes it.
I have to admit, I've never eaten anything with a name like "GemTec 1160" and the name made me suspicious. If they used "Bob's Vital Wheat Gluten" or something like that I probably wouldn't have put so much effort into figuring this out.
I also saw that many of the company's wheat gluten products were treated enzymatically, and I wondered whether some might be treated with tissue transglutaminase, since the food industry often uses this enzyme and at least sometimes, as in the case of Japanese noodles, actually treats wheat with it. So I asked the corresponding author listed on the study, who responded very politely and very professionally but not very helpfully. After all, the investigators had no idea how the gluten was treated and suggested I contact the company.
So I did. A representative of the company told me that although he couldn't divulge the specifics, GemTec 1160 is a "chemically modified protein" that is "definitely deamidated."
So it turns out that this "gluten" is the type of gluten you'd find in the intestine of someone with celiac disease, who has been mis-behaving and eating all sorts of bread. The type of gluten you'd only find after they ate it.
(Of course, the specific digestive pattern might be different, but the deamidation is the same.)
So unfortunately, while the study was well controlled, it's not entirely clear that its findings are relevant to anyone eating bread, as bad as most bread may be. Providing they aren't having a friend with celiac disease eat it first.
That said, let's take a closer look at what the study actually found.
First, they recruited people who had already decided to go gluten-free. These were people who were already convinced they had a problem with gluten. This makes the study very vulnerable to a placebo effect. Or, more accurately, a nocebo effect.
Thankfully, the investigators not only used a placebo control, but even assessed the efficacy of that control by asking the subjects to guess which group they were in. This is a sign of a high-quality study performed by conscientious and rigorous scientists. The authors reported a statistical analysis that suggested the blinding was effective, but the corresponding author did helpfully inform me that 58 percent of the subjects correctly guessed their group. This is hardly better than tossing a coin.
The authors, however, reported no details about how they tested blinding efficacy. Ideally, the investigators would urge the subjects to report the truth rather than an answer they consider socially acceptable, and would give them the option of saying they didn't know which group they were in, or even rating their confidence about which group they belonged to if they were guessing. In a truly successful blinding, most of patients would honestly state that they didn't know what group they were in. This is quite different from having everyone guess and finding that the proportion of people who guessed correctly is not statistically significantly higher than half.
Ineffective blinding does not necessarily invalidate a study's conclusions, because it could have been the intestinal symptoms that gave away the blinding rather than the taste of the muffins. That is why it is best to also include a question about why the subjects thought they were in a particular group in the questionnaire. In a study of the role of fish oil in depression where 60 percent of the participants guessed correctly whether they were in one group or the other based on the taste of the capsules, we'd be much less convinced than if they guessed correctly based on whether their depression improved. The same principle operates in this study, but we don't have any of these details.
Fifty-eight percent may not be statistically better than a coin toss if people are forced to guess one way or the other, but it's certainly enough people to bias the results in one direction in the placebo group and in the opposite direction in the gluten group, if there is in fact a placebo or nocebo effect going on.
And that is particularly concerning because there was no biochemical evidence to back up the self-reported symptom ratings.
There were no changes in serum antibodies to gluten, C-reactive protein (a marker of inflammation), or intestinal permeability.
Granted, this in no way rules out that the chemically processed, deamidated gluten had a real effect. These markers are very limited and there could have been a real effect mediated by innumerable other pathways. And a recent paper by gluten researcher Dr. Allesio Fasano and colleagues recently concluded that people whom the investigators judged to be gluten-sensitive but without celiac or wheat allergy actually had reduced intestinal permeability.
This certainly contradicts the idea that zonulin-mediated intestinal barrier dysfunction has any relevance to non-celiac gluten sensitivity, but it also makes it clear that the inability of the Australian study to show a change in intestinal permeability in no way invalidates their findings or proves that all they discovered was a nocebo effect.
Nevertheless, the way that the authors present their data is rather frustrating and it is difficult to disentangle just how much of an effect there actually was.
The main endpoint was "the proportion of patients answering 'no' on more than half of the symptom assessments to the question, 'Over the last week were your symptoms adequately controlled?'" They asked this question for each of the six weeks of the study.
But here is how they reported the data for their main endpoint:
Significantly more patients in the gluten group (68%; n=13/19) reported the answer, “no” (the primary outcome question) compared with those on placebo (40%; n=6/15) for more than half of the study therapy duration (P=0.001; generalized estimating equation).
The first disturbing thing is that there was a very high rate of people who did not have their symptoms under control in both groups. But the most frustrating thing is that the authors do not report the raw data and we have no idea who had these symptoms under control at the start of the study, nor whether the groups became more divergent or more similar over the study period.
If few people at the beginning of the study answered no, this number increased over time in the gluten group, and the difference between the gluten and placebo groups continued to diverge over the duration of the study, this would be quite convincing. If the rate of answering "no" was high to begin with, and if the difference between groups was greatest in the first half of the study but diminished over time, this would not be very convincing at all.
Likewise, they reported increased severity of symptoms in both groups, but a greater increase in the gluten group. They never reported the actual values, so it is impossible to judge whether this is likely to be a true effect or likely to be regression to the mean — the tendency for extreme values to gravitate towards "average" values over time.
In order to make the differences in change from baseline meaningful, we would want assurance that symptom severity was similar between the two groups at baseline, and we would also want assurance that the absolute severity of the symptoms and not just their change from baseline was also different by the end of the study. Unfortunately, this report does not provide that assurance.
Overall, I am left with the following impressions from the study:
While the study was well controlled, the data were not thoroughly reported and it is difficult to tell how convincing the effects are.
The possibility that many people knew which group they were in raises concerns about a nocebo effect, which is the opposite of a placebo effect.
The failure to corroborate any of the self-reported symptoms with biochemical evidence further supports concerns about a nocebo effect.
The fact that many people reported poor control of symptoms during the study even in the placebo group and that symptoms worsened in both groups suggests either a nocebo effect or a harmful effect of the gluten-free bread and muffins, both of which are very plausible.
The relevance of chemically deamidated gluten to someone without celiac who is eating bread is highly questionable.
Despite these imperfections, this study is encouraging because it shows that rigorous experimental evidence can and will be used to investigate the possibility of non-celiac gluten sensitivity. Now we can begin to move away from cell culture studies with questionable physiological relevance and move into studying the real effects of gluten in live people. This study marks a milestone in non-celiac gluten sensitivity research and shows that the quality of research is increasing.
The relevance of gluten to people's apparent intolerance to wheat remains an open question that deserves and needs more attention and investigation.
I will eventually write a more in-depth post about wheat in my series on food toxins and food intolerances. In the mean time, I have a few quick observations:
People who react to gluten are likely to have an equal or worse problem with white bread than with whole grain. White bread should have a greater proportion of gliadin than whole grain bread.
You can probably best test whether you react to wheat germ agluttinin by trying wheat germ, as it would be most concentrated in this fraction.
If you react to wheat bran, this would seem to implicate the fructans, or at least some portion of the fiber. Fructans are present in whole flour at similar concentrations, but at least the bran has less of the other confounders. If you react to onions and other foods high in fructans, this is also supportive. However, different foods have fructans of different chain lengths, and these different fructans could affect people differently.
Gliadin ("gluten") is sort of a non-specific lectin that binds a number of different sugars including mannose polymers, N-acetyl-glucosamine, galactose, arabinose, and rhamnose. Wheat germ agglutinin is specific for N-acetyl-glucosamine, but also reacts with galactose. I have talked to a few people who found that supplementing with these sugars help them tolerate gluten. While this is not going to provide a very specific test and should be considered quite speculative, if supplementing with these sugars proves helpful, this would seem to make it more likely that gliadin or wheat germ agglutinin is the culprit.
I'm definitely looking forward to reading more of the Gluten-Free January results, and I'm excited to see more and more direct research in humans coming out on this issue. This should prove to be a good year for understanding more about wheat.
Read more about Chris Masterjohn, PhD, here.